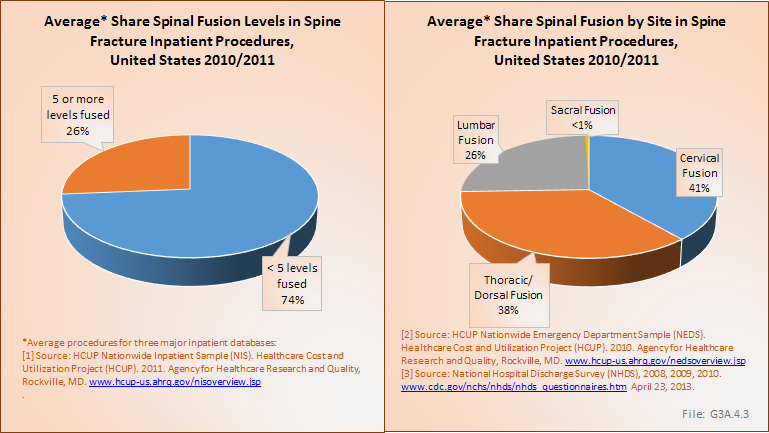
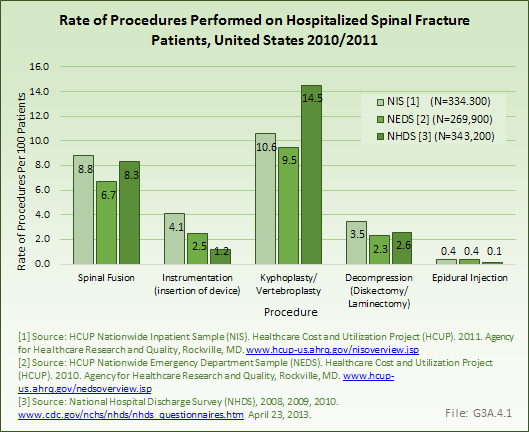
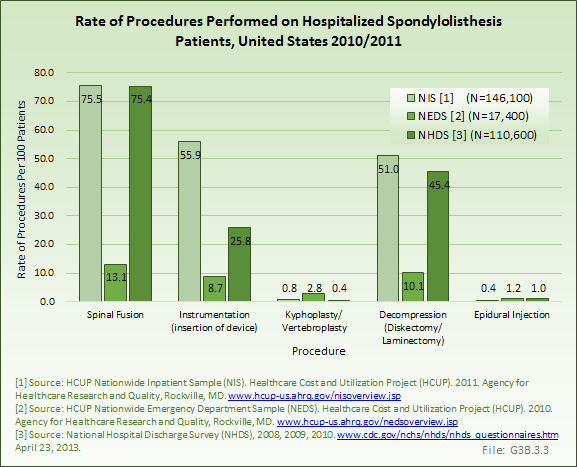
Many patients with spondylolisthesis have no symptoms, and most likely do not require any significant treatment or intervention. Symptomatic patients are most frequently treated nonsurgically with NSAIDs, activity modification, physical therapy, and possibly epidural steroid injections. Bracing may be appropriate in some patients, particularly children with acute lesions.1,2 Surgical treatment is indicated when patients have significant disabling pain despite 6 months of adequate nonsurgical care or, less commonly, a progressive lesion. Treatment typically involves a posterior lumbar fusion. Instrumentation is thought to improve the fusion rate and clinical outcome,3 and decompression is included for patients with stenosis and associated radicular leg symptoms. Reduction of slips of greater than 50% remains controversial, but is thought to correct kyphosis and global sagittal balance, decrease the length of fusion, and protect against adjacent segment degeneration.4,5
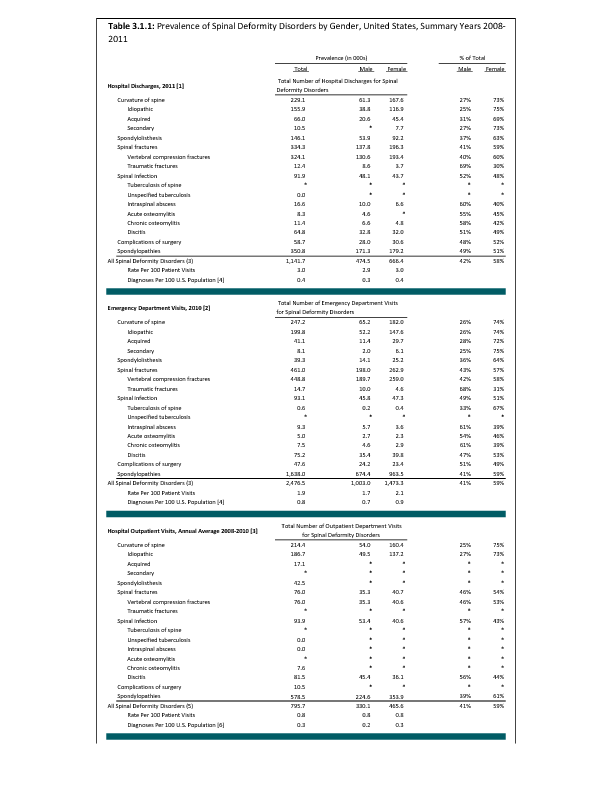
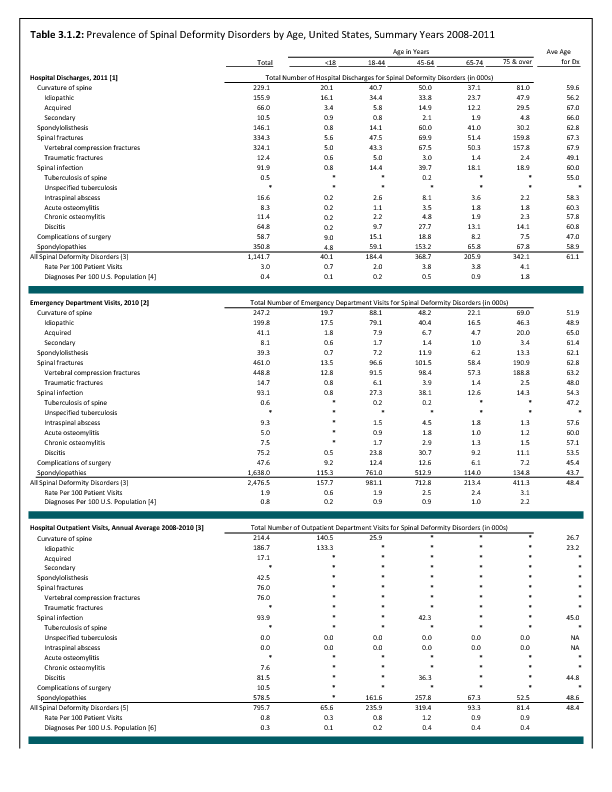
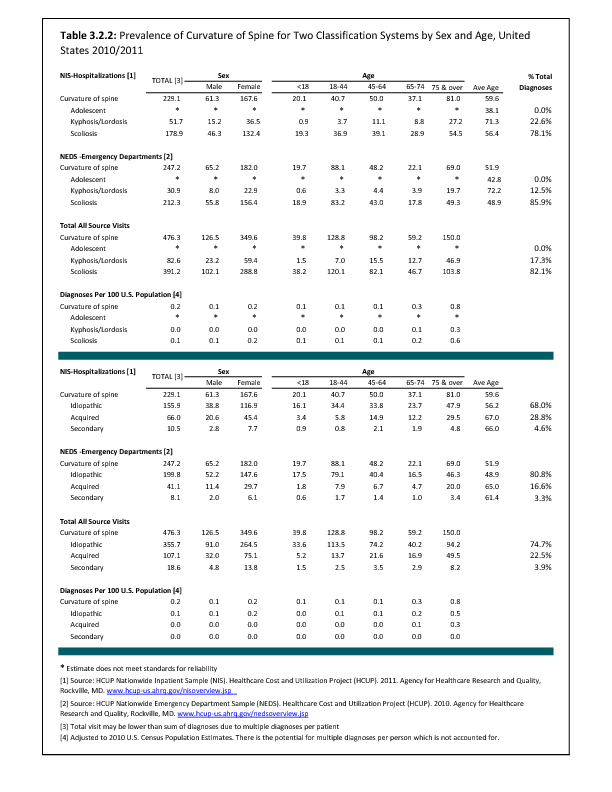
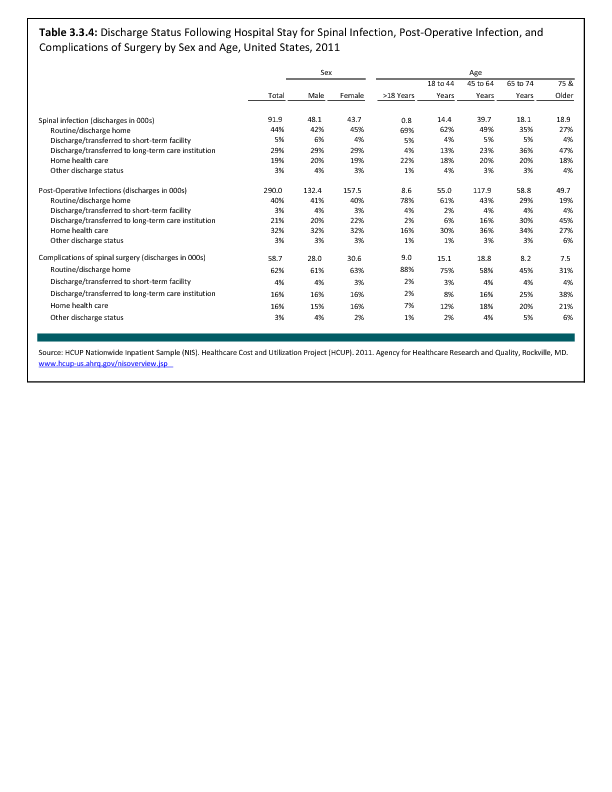
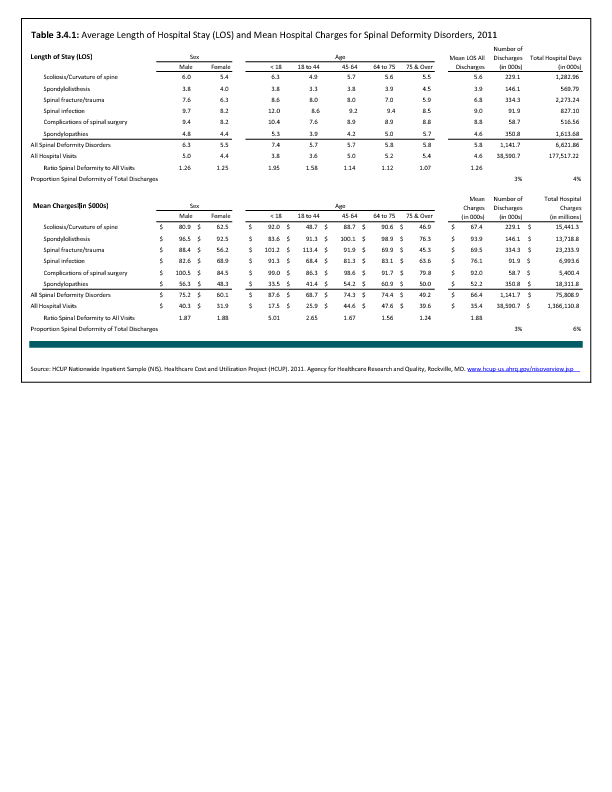
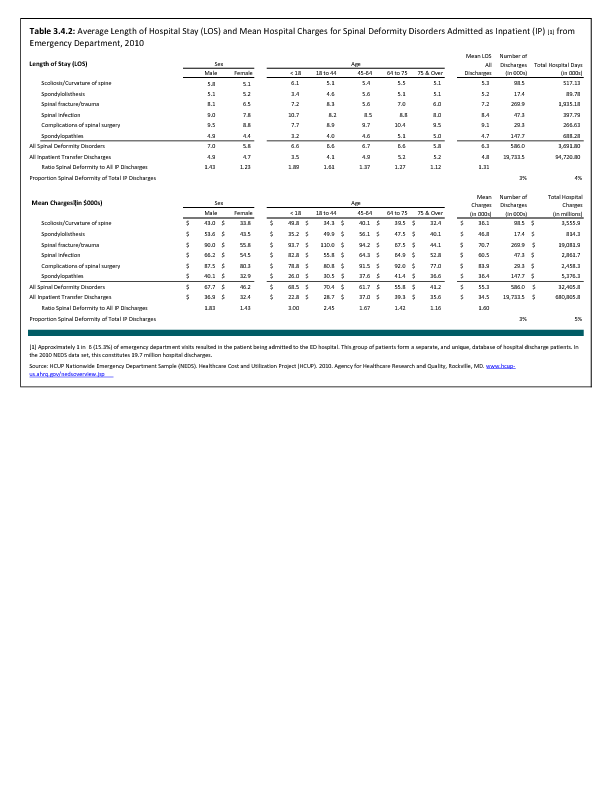
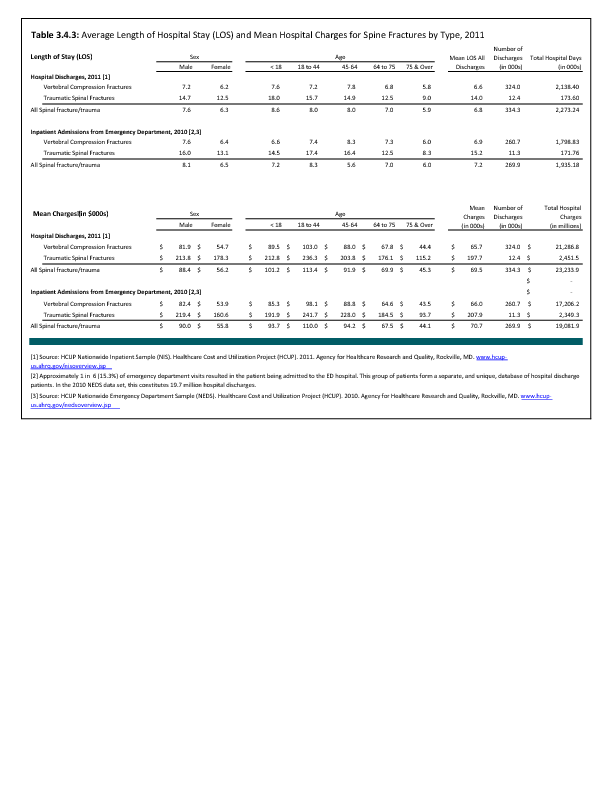
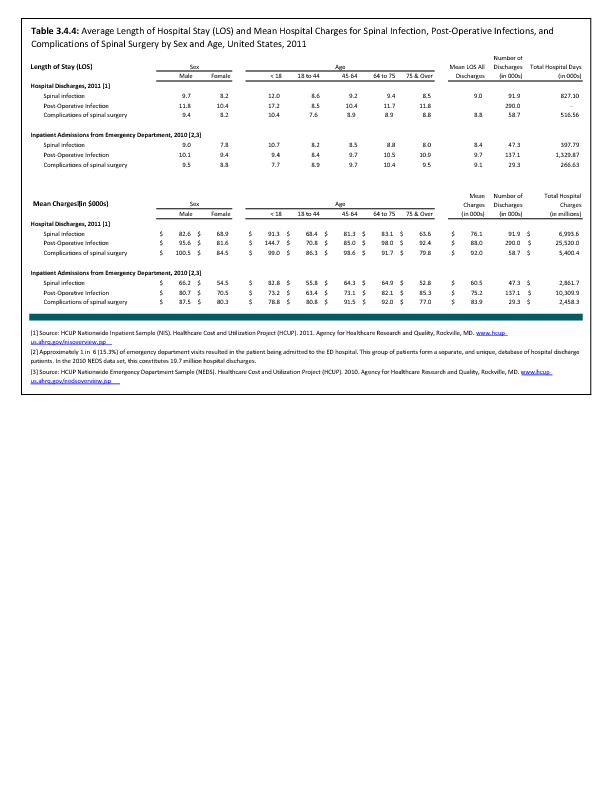
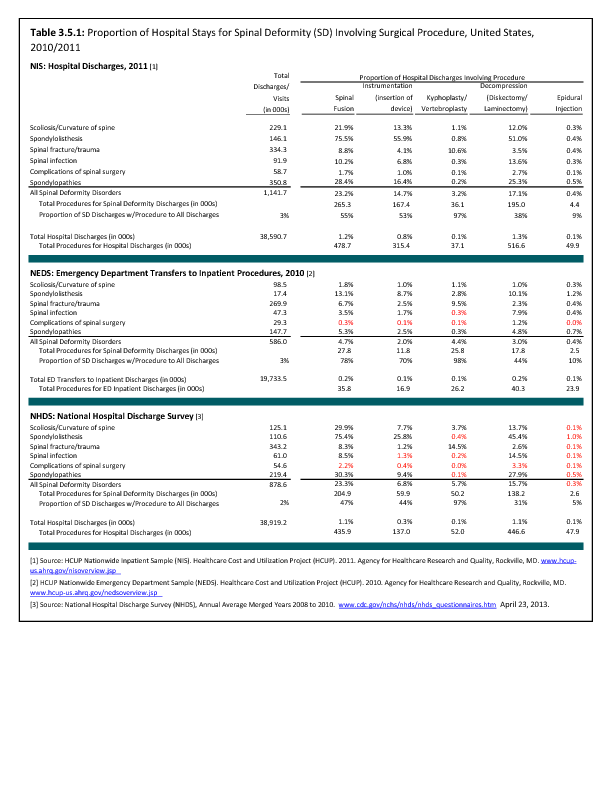
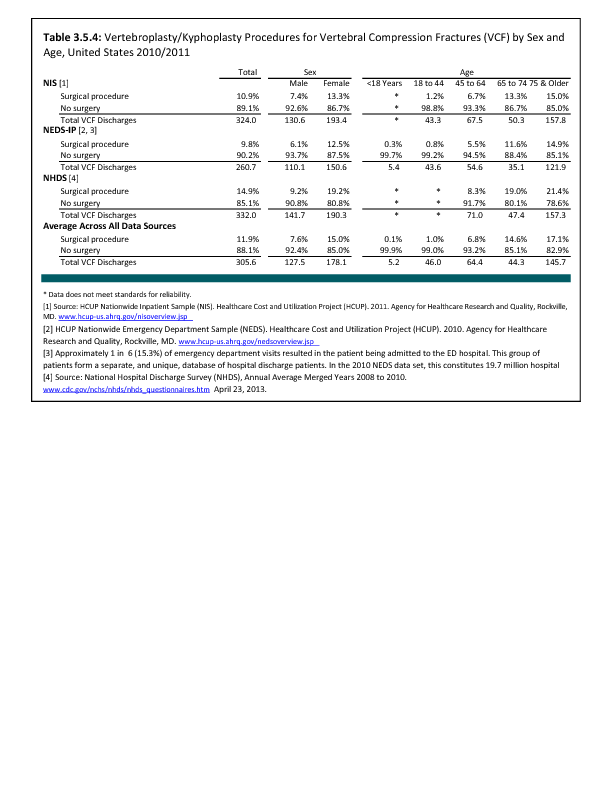
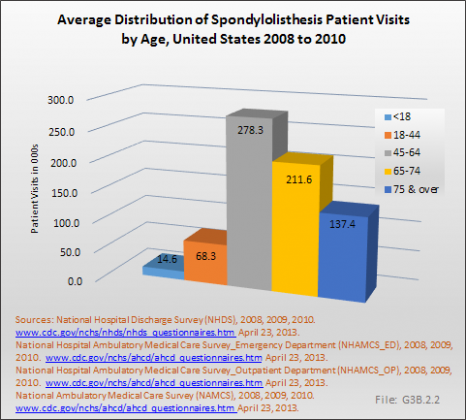
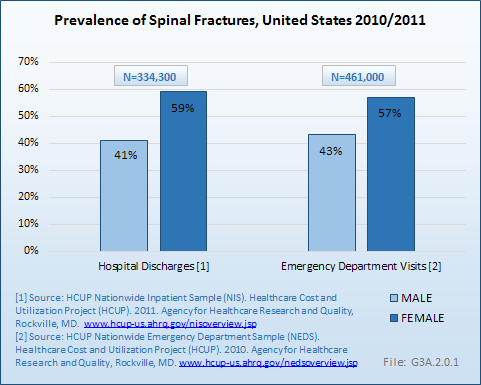
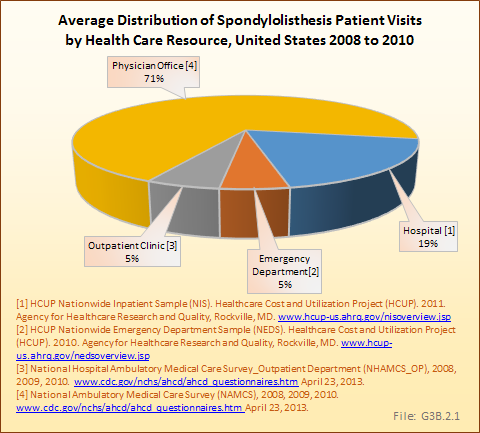
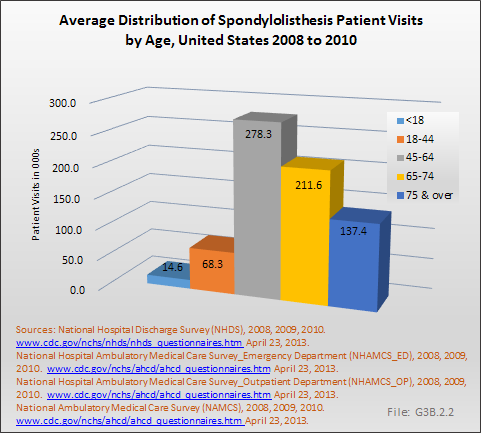
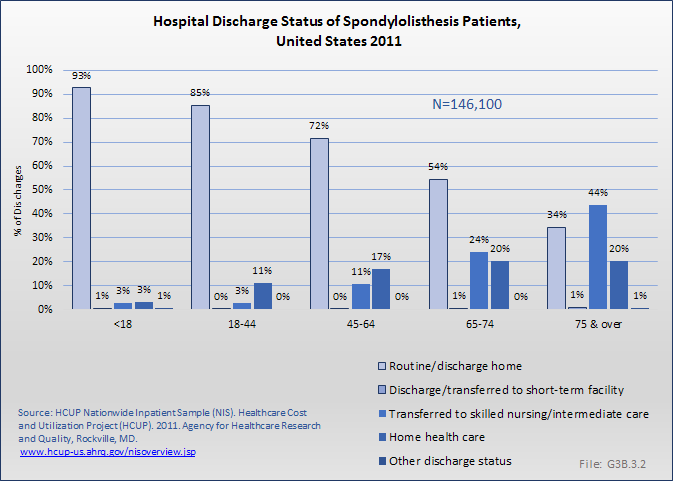
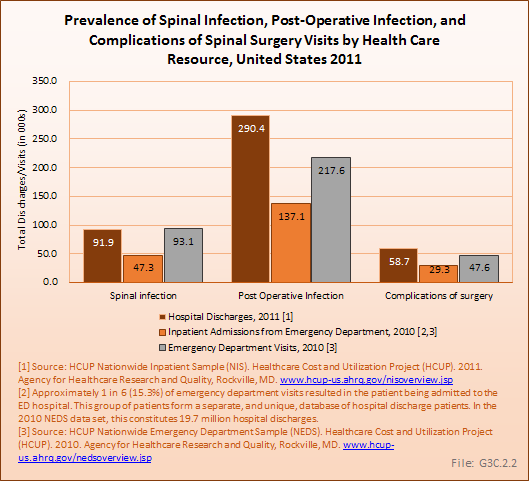
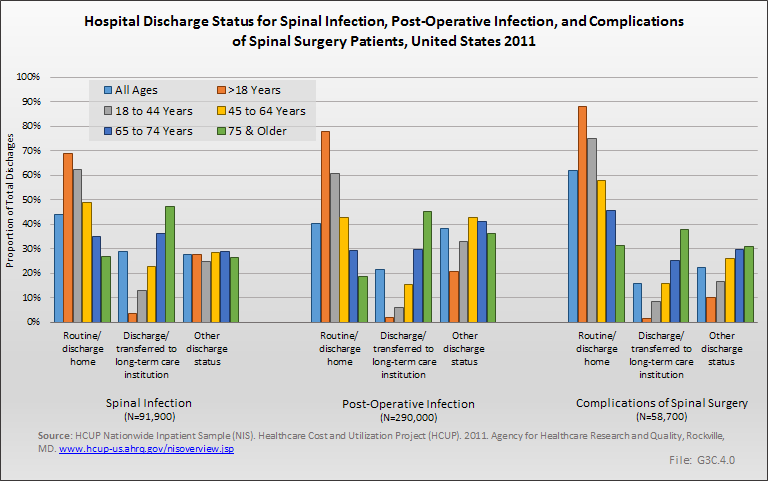
Analysis of various inpatient and outpatient databases from 2008–2011 showed 778,700 visits with a diagnosis for spondylolisthesis. The majority of these visits (81%) were outpatient visits, primarily to a physician office. More than two in three (69%) visits for spondylolisthesis were by females with an average age between the late 50s or early 60s. More recent data from 2010–2011 demonstrate 185,400 hospital or emergency department discharges for spondylolisthesis with similar age and sex distribution (Reference Table 3.1.1 PDF CSV and Table 3.1.2 PDF CSV).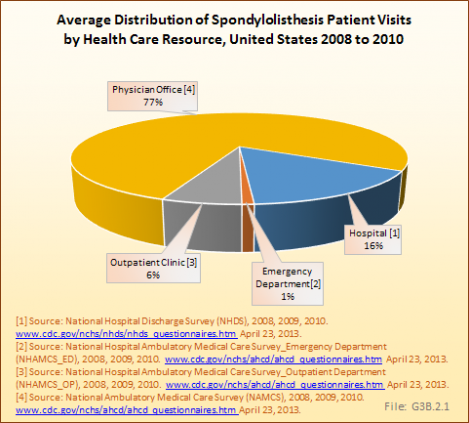
- 1. Hu SS, Tribus CB, Diab M, et al: Spondylolisthesis and spondylolysis. J Bone Joint Surg Am 2008;90(3):656-671.
- 2. Steiner ME, Micheli LJ: Treatment of symptomatic spondylolysis and spondylolisthesis with the modified Boston brace. Spine 1985;10(10):937-943.
- 3. Zdeblick TA: A prospective, randomized study of lumbar fusion: Preliminary results. Spine 1993;18(8):983-991.
- 4. Transfeldt EE, et al: Evidenced based medicine analysis of isthmic spondylolisthesis treatment including reduction versus fusion in situ for high grade slips. Spine 2007;32(19 suppl):S126-S129.
- 5. Hu SS, Bradford DS, Transfeldt EE, Cohen M: Reduction of high grade spondylolisthesis using Edwards instrumentation. Spine 1996;21(3):367-371.
Edition:
- 2014











 Download as CSV
Download as CSV