

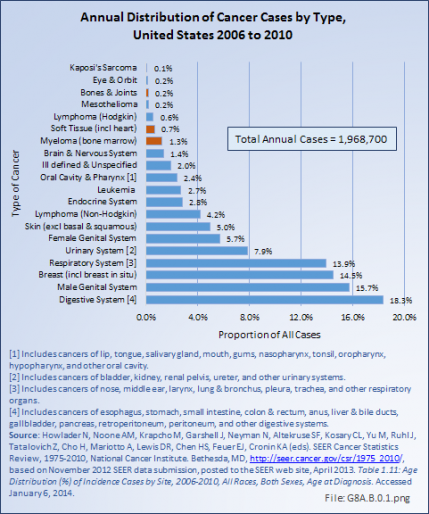
Bone and connective tissue neoplasms, which include bone and joint sarcoma, myeloma, and soft tissue sarcomas, are uncommon when compared with other cancers and with other musculoskeletal conditions, accounting for about 2.2% of annual cancer cases between 2006 and 2010 (approximately 43,000 cases). This is slightly higher than the rate of 1.9% reported previously for the years 2002 to 2006. The annual average number of new bone and joint cancer cases between 2006 and 2010 was 3,888, while during this same time an average of 1,360 deaths from bone and joint cancer occurred each year. (Reference Table 8A.1.1 PDF [1] CSV [2], Table 8A.3.1 PDF [3] CSV, [4] and Table 8A.3.3 PDF [5] CSV [6])
Data from the Surveillance Epidemiology and End Results (SEER) [7] program of the National Cancer Institute, used to present the burden of bone and connective tissue neoplasms, is the most comprehensive source of information on cancer incidence, prevalence, mortality, survival, and lifetime risks. Data is currently available from 1974 to 2006. The SEER program is one of the most comprehensive sources of neoplasm data; it is based on data representing approximately 10% of the US population.
In addition, data from the American College of Surgeons’ Commission on Cancer National Cancer Data Base (NCDB) [8] was used in the analysis for staging and growth rates for common cancers. The NCDB is maintained by the American College of Surgeons, containing much of the same standardized data as that collected by the SEER database. Data are collected from all institutions wishing to be accredited by the American College of Surgeons Commission on Cancer. Each accredited institution is required to report all patients with cancer treated at their institution, including annual follow-up data. Site visits and interaction between American College of Surgeons cancer database personnel and the local reporting institutions verifies a minimum of 90% case capture and reporting for each institution. Multiple internal checks verify the data accuracy. It is estimated that the approximately 1,500 reporting institutions each year treat approximately 71% of all patients with malignancies in the United States. The primary author was granted research access to the database under the Participant User File (PUF) research program. However, accessible data was only for cases in patients 18 years old and older, showing the age-related aspects of the NCDB dataset.
The three most common primary cancers of bones and joints are osteosarcoma, Ewing sarcoma, and chondrosarcoma. Of the three, chondrosarcoma has the best prognosis. The ages at which these cancers most often occur vary. Osteosarcoma, a malignant bone tissue tumor commonly found near the growing end of the long bones, is the most common, and occurs most frequently in teens and young adults. Ewing sarcoma, a tumor often located in the shaft of long bones and in the pelvic bones, occurs most frequently in children and youth. Chondrosarcoma, a sarcoma of malignant cartilage cells, often occurs as the result of malignant degeneration of pre-existing cartilage cells within bone, including chondromas (a benign tumor), and is primarily found among older adults. However, the vast majority of chondromas never undergo malignant change; therefore, the routine resection of benign chondromas is unwarranted.
Of these three, Ewing sarcoma is generally considered to have the worst prognosis, followed by osteosarcoma. However, this perception is largely due to the greater tendency for osteosarcomas to present as high-grade tumors and for chondrosarcomas to present as low-grade tumors. When analyzed by stage, a recent survivorship analysis revealed similar survivorship rates for low-grade chondrosarcoma compared to low-grade osteosarcoma, and similar survivorship rates for high-grade chondrosarcoma when compared to high grade osteosarcoma. By definition, all cases of Ewing sarcoma are high-grade, the most aggressive category of cancer, with full potential to metastasize and bring about death. Approximately 6% to 20% of osteosarcomas are of lower grade; chondrosarcoma has a higher proportion of low-grade cases than these other two bone and joint cancers.
The fourth common “primary” cancer of the bone is myeloma, a malignant primary tumor of the bone marrow formed from a type of bone marrow cells called plasma cells (the cells that manufacture antibodies). This cancer and usually involves multiple bones simultaneously. The isolated single-bone version of myeloma is called plasmacytoma, but virtually all cases of isolated plasmacytoma evolve into full-fledged multiple myeloma within 5 to 10 years after diagnosis of the plasmacytoma. Like leukemia and lymphoma, myeloma is more properly considered a primary cancer of the hematopoietic bone marrow. Unlike leukemia, however, myeloma typically causes extensive changes or damage to the bone structure itself, causing fractures, pain, and hypercalcemia. Because of the associated bone destruction, myeloma is generally included in analysis of bone cancers; however, leukemia and lymphomas generally are not considered primary bone cancers, presumably because of the lower likelihood of structural bone destruction and associated complications. Non-Hodgkin’s lymphomas, however, warrant some consideration due to the frequency of bone destruction and pathological fractures requiring operative intervention.
SEER estimated that in 2013, 3,010 people were newly diagnosed with cancer of the bones and joints. The number of new cases of bone and joint cancers is 0.9 per 100,000 people per year. In addition, 1,440 people will die annually from cancer of the bone and joints.1 According to SEER statistics, the rates for new bone and joint cancer cases have been rising, on average, 0.4% each year over the last ten years. However, death rates have fallen on average 0.3% per year, with survival rates rising slightly. Incidence estimates derived from NCDB are slightly higher without an appreciable change in survival. There has been a gradual increase in the number of cases reported to the NCDB in the past 13 years. While the reason for this difference is unknown, it could reflect reporting changes rather than incidence changes.
Myeloma occurs five to six times as frequently as the other bone cancers. It will be diagnosed in 22,350 persons per year, an incidence rate of 5.9 per 100,000 persons per year. An expected 10,710 persons died of myeloma in 2013.2
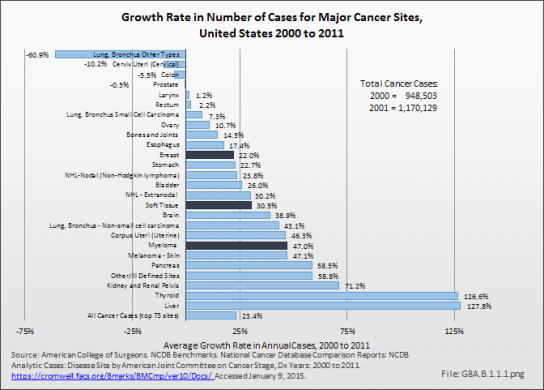
Although annual cases included in the American College of Surgeons National Cancer Data Base (NCDB) show a slower rate of increase, proportionately, for bone and joint cancers than for cancer cases overall, the incidence of bone and joint cancers is increasing. Between 2000 and 2011, the annualized number of primary cases recorded increased by nearly 15%. Myeloma cases, however, increased at twice the rate of cancer cases overall, 47% to 23%, respectively. (Reference Table 8A.5.2 PDF [9] CSV [10])
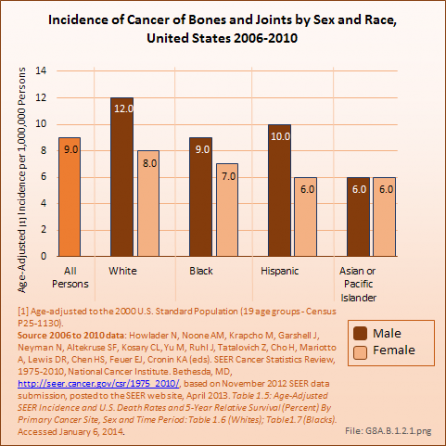
Gender and Race
Bone cancers and soft tissue sarcomas are found more frequently in males than females, and more frequently among Whites than those of any other race. However, rates have varied slightly for both genders and by race for the past decade. The average annual incidence of bone cancers between 2006 and 2010 was nine in one million, a rate that has remained constant for the last decade. The rate among White males was 12 in one million, while, among White females it was eight in one million. The lowest rate of six in one million was found for both males and females of the Asian or Pacific Islander race. The incidence of cancer of the bones and joints in the United States is comparable to several site-specific oral cancers (ie, lip, salivary gland, floor of the mouth), cancers of the bile duct, cancers of the eye, and Kaposi’s sarcoma, which affects the skin and mucous membranes and is often associated with immunodeficient individuals with AIDS. (Reference Table 8A.1.1 PDF [1] CSV [2])
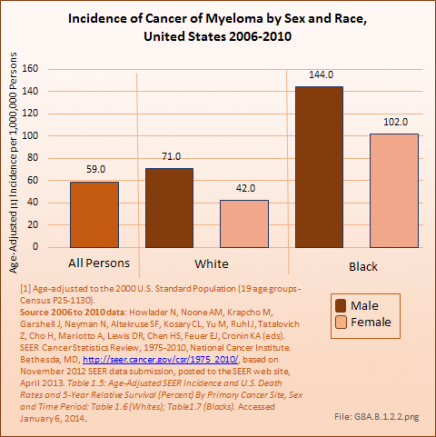
As with bone and joint cancers, males have a higher incidence of myeloma than do females, with an average of 71 cases in one million males to 42 cases in one million females. Blacks have a much higher incidence rate of myeloma than Whites. The incidence of myeloma in the United States is comparable to the incidence of esophageal, liver, cervical, ovarian, brain, and lymphocytic leukemia cancers. (Reference Table 8A.1.2 PDF [13] CSV [14])
Age
The median age for cancers of the bones and joints has risen slightly, to age 42 years, in recent years. However, it remains the leading cause of cancer in young persons under the age of 20 years. More than one in four diagnoses of bone and joints cancer is in children and youth under the age of 20 years, with more than one-half (52%) of cases diagnosed in person younger than 45 years. Males are typically diagnosed with bone cancers, and die from bone cancer, at an age several years younger than females. (Reference Table 8A.2.1 PDF [15] CSV [16] and Table 8A.3.2 PDF [17] CSV [18])
Myeloma, on the other hand, is primarily a cancer found among elderly persons, with a median age of 69 at the time of diagnosis. Eight-five percent of new myeloma cases are diagnosed in persons age 55 years and older. Again, males are typically diagnosed with myeloma at ages several years younger than females. (Reference Table 8A.2.1 PDF [15] CSV [16], Table 8A.2.2 PDF [19] CSV [20], and Table 8A.3.2 PDF [17] CSV [18])
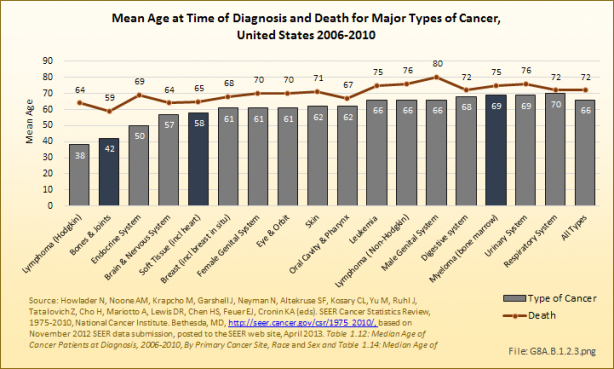
Death from bone and joint cancer, at a median age of 59 years, occurs at a younger age than any other type of cancer. (Reference Table 8A.2.2 PDF [19] CSV [20])
Annual population-based mortality rates due to cancers of bones and joints are low, averaging four deaths per one million people since the early 1990s.1 While the mortality rate from bone and joint cancer dropped by approximately 50% from that of the late 1970s, no significant improvement in this rate has been observed over the past 20 years.2 Males have a higher mortality rate than females for all races. (Reference Table 8A.4.3 PDF [21] CSV [22])
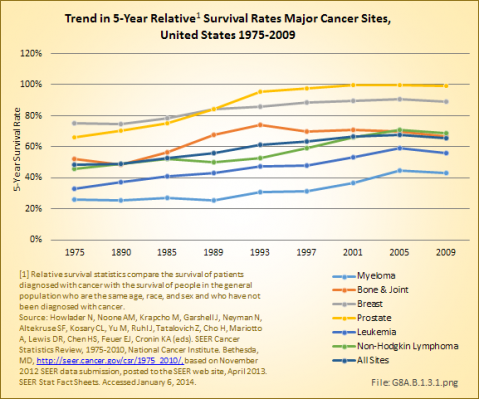
The overall 5-year survival rate in 2006–2010 for bone and joint cancers was 66%, placing it roughly in the middle of all cancers for 5-year survival and comparable to a number of more common cancers such as non-Hodgkin lymphoma, urinary, cervical/ovarian, and soft tissue cancers. This is an increase of 14% since 1975, when the 5-year survival rate was 52%. The median number of years of survival after diagnosis is 17, with males averaging 16 years and females 18 years.
The overall 5-year survival rate for the primary types of bone and joint cancers is 54% for osteosarcoma, 75% for chondrosarcoma, and 51% for Ewing sarcoma. The osteosarcoma survival rate varies with age: The 5-year survival was 70% for children and youth under the age of 20 years,3 60% for people under 30 years of age, 50% for those aged 30 years to 49 years, and 30% for those 50 years old and older.2 If Ewing sarcoma is found before it metastasizes, the 5-year survival rate for children and youth is about 70%. However, if already metastasized when found, the 5-year survival rate drops to 15% to 30%.4 (Reference Table 8A.4.1 PDF [23] CSV [24], Table 8A.4.2 PDF [25] CSV, [26] and Table 8A.4.3 PDF [21] CSV [22])
The annual population-based mortality rate of myeloma was an average of 34 persons per one million population between 2006 and 2010.5 The mortality rate from myeloma has remained relatively constant since the mid-1970s. The 5-year survival rate for myeloma, 43%, is one of the lowest for all cancers; however, due to being primarily a cancer of older persons, this age-relatedness may well affect survival regardless of the presence or absence of myeloma. The median survival after diagnosis of myeloma is only 6 years. (Reference Table 8A.4.1 PDF [23] CSV [24], Table 8A.4.2 PDF [25] CSV, [26] and Table 8A.4.3 PDF [21] CSV [22])
Within the NCDB, no change in the overall survival rates for patients diagnosed and treated in the years 1985 to 1988 compared to patients between 1994 and 1998 was found. There have been no substantial changes in therapies utilized for osteosarcoma since 1998 and the overall 1998–2010 NCDB data reveals no significant improvement, with an approximate 50% five-year overall survival. However, the survival rate varies greatly with the histologic subtype of sarcoma. For instance, the 5-year relative survival rate is 53% for classic high-grade osteosarcoma, 87% for parosteal osteosarcoma and 18% for osteosarcoma associated with Paget's disease of the bone. (Reference Table 8A.8.1 PDF [27] CSV [28])
The economic burden of bone cancers can be great. The more advanced the disease, the worse the prognosis and, accordingly, the more expensive the treatments. It is likely that early detection, and, certainly, prevention if possible, could drastically reduce costs. A number of expensive treatments are required to address these tumors. In the 2007 report by Damron, Ward, and Stewart,1 it was noted that the most frequent initial treatments varied widely based on the type of sarcoma. Although not reported, these treatments vary widely based on the stage of the disease as well.
Collectively, they reported that surgery alone was the most common initial treatment for chondrosarcomas (69%), whereas for Ewing sarcoma, treatments were divided between surgery and chemotherapy (24% of cases), radiation and chemotherapy (23%), and chemotherapy alone in 18%. With osteosarcoma, when initial treatment was known, the largest group received surgery and chemotherapy (46%). Surgery was reported as part of the initial treatment in 71% of osteosarcoma patients, 83% of chondrosarcoma patients, and 47% of Ewing sarcoma patients. The most frequent operations performed were limb-sparing radical resections and excisions. When the type of surgery was defined and known, limb-preservation surgery was performed in 69% of osteosarcomas, 79% of chondrosarcomas, and 81% of Ewing sarcomas.1
Radiation therapy was employed in 10% of osteosarcomas, 14% of chondrosarcomas, and 46% of Ewing sarcoma cases. In Dr. Ward’s personal series of more than 100 osteosarcomas, amputation has been required in only 17% of patient, but almost all patients have had surgical resection, limb reconstruction, and chemotherapy.1
Multiple therapies may be needed later in the course of the patient’s disease, especially in the more advanced cases. In later stages of the disease for those not cured with surgery alone, significant costs will accumulate as the patients develop pulmonary disease and, ultimately, die. Hormone therapy, immunotherapy, and bone marrow transplant/endocrine treatments each accounted for 1% or less of initial treatments. However, in severely affected individuals in whom standard treatments fail, these alternative treatments may be tried more frequently. Currently, the authors are not aware of any data source that reports the rate of utilization of such late treatments.
All of these treatments are costly to administer. Per-patient cost will vary widely depending on the treatments utilized, and the number and intensity of treatments. Over all, treatment for bone and joint cancers can easily exceed $100,000 for a single patient. This is particularly true if that patient receives surgery, chemotherapy, and radiation therapy. If one includes the cost of bone-replacing endoprostheses or the costs of artificial limbs used in those cases that required amputations, the cost will be much higher. In addition to the direct medical cost, there are extensive indirect and social costs from lost work time and disability. For some patients, healthcare costs associated with their bone and joint cancers will be ongoing.
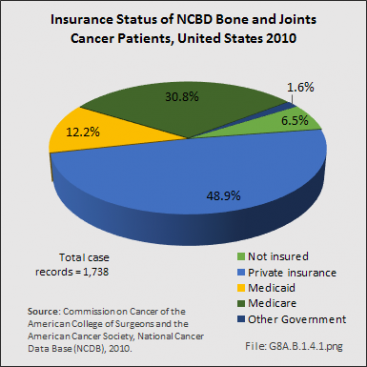
The burden of paying the cost of treatment for bone and joint cancers is shifting. In the study cited above, from 1998 to 2010, managed care provided insurance coverage for the largest portion of patients (37%), following by Medicare with supplement (16%). Medicare and Medicaid were roughly equal at 8% and 8%, respectively. However, analysis of the NCDB insurance data available for 1,738 (95.7%) of 1,816 bone and joint cancer cases reported for 2010 show Medicare and Medicaid covering a much larger share.
Almost all cancers have preferential sites to which they spread or metastasize, resulting in secondary cancers. Secondary bone cancer is much more common than primary bone cancers, and result in great morbidity and pain. The three most common sites of cancer metastasis are lung, liver, and bone. The skeleton is the most common organ affected by metastatic cancer, and the site of disease that produces the greatest morbidity. The most commonly encountered cancers that readily and frequently spread to bone are cancers of the breast, lung, kidney, prostate, gastrointestinal tract, and thyroid gland. The incidence of bone metastases in lung cancer patients is approximately 30% to 40%, and the median survival time (MST) of patients with such metastases is 6 to 7 months.1 At postmortem examination, 70% of patients dying of breast and prostate cancer have evidence of metastatic bone disease. Cancers of the thyroid, kidney, and bronchus also commonly give rise to bone metastases, with an incidence at postmortem examination of 30% to 40%.2 Brain and ovarian cancers rarely spread to bone. Many other cancers have intermediate rates of spread to bones.
A tumor formed by metastatic cancer cells is called a metastatic tumor or a metastasis. The cancer cells in their new metastatic site closely resemble the original or primary cancer from which the cancer initially arose. For example, breast cancer that spreads to the bone and forms a metastatic tumor is still considered metastatic breast cancer, not true bone cancer. It will still look like breast tissue and breast cancer when it is inspected or viewed under a microscope. Many lay people will now refer to it as bone cancer, but to the physician, bone cancer implies a cancer that started or originated in the bone, such as osteosarcoma, Ewing sarcoma, or myeloma, as discussed above.
Metastatic bone disease complications are termed skeletal-related events (SREs). SREs include pain, pathologic fracture, vertebral deformity and collapse, spinal cord compression, and hypercalcemia (overabundance of calcium in the blood) of malignancy. These complications result in impaired mobility and reduced quality of life (QOL) and have a significant negative impact on survival.2 In addition, metastatic disease may remain confined to the skeleton, with the decline in quality of life and eventual death almost entirely due to skeletal complications and their treatment.
The prognosis of metastatic bone disease is dependent on the primary site, with breast and prostate cancers associated with a survival measured in years compared with lung cancer, where the average survival is only a matter of months. Survival rates for secondary bone cancer depend on patient factors such as age, overall health, treatment, and response to treatment. However, due to the advanced stage of cancer that has spread, survival rates are much lower than for primary cancer without such spread.
The fundamental treatment for bone metastasis from advanced cancer is disease control by systemic chemotherapy and radiation of the bone lesions. Prevention and treatment of bone metastases is highly dependent on an effective treatment being employed against the primary cancer. As a direct treatment for bone metastases themselves, radiation therapy, surgery, and bisphosphonates are the mainstays of treatment. Intravenous bisphosphonates, such as zoledronic acid have been shown to prevent or reduce pathologic fractures and may reduce these costs.3 With FDA approval of the use of bisphosphonate medications to prevent such fractures in 1995, the incidence of fractures in treated patients has significantly decreased. The fracture rates reported in cases of metastatic disease and myeloma have been demonstrated in multiple studies to markedly diminish (roughly a 50% reduction in fracture rates in many studies). Although the tumors still metastasize to the bone, the associated bone destruction and consequent pathologic fracture rate is markedly less. The bisphosphonate medications work by interrupting a biochemical pathway required for bone breakdown by osteoclasts, the cells that normally remove bone in the process of bone remodeling. This bone breakdown step is overactivated in the presence of bony metastases, causing bone loss, bone destruction, and ultimately fractures from the weakening of the bone. Thus, the introduction of bisphosphonate medication has been a major advance over the past 20 years, one that had significant impact on the health of those with myeloma and metastatic cancer to the bone by preventing bone destruction, and thereby preventing bone weakening and subsequent fractures.
The economic burden of SREs in patients with bone metastases is substantial. A recent study showed that the estimated lifetime SRE-related cost per patient suffering from metastatic lung cancer was $11,979 USD, and that radiotherapy accounted for the greatest proportion of cost (61%) by SRE type.1 Finding cures and effective treatments for all types of cancer can help reduce the prevalence and costs associated with bone and joint cancer.
Overall cancers metastatic to bone cause significant pain and morbidity—approximately 50% of patients with metastatic cancer of lung, breast, prostate, and kidney develop bony metastases prior to death. Untreated, these metastases can lead to pathological fractures and cause great pain and disability. Thus, the elucidation of the biochemical steps involved in bone destruction and the development of drugs to combat such steps, have been an example of tremendous scientific advancement and achievement in the field of cancer research and treatment.
Soft tissue tumors, which, like bone tumors, are also called sarcomas, are encountered more frequently than bone and joint tumors. These tumors originate in connective or non-glandular tissue, and can develop in any part of the body that contains fat, muscle, nerve, blood vessels, fibrous tissues, and in any deep tissues, including tissues surrounding joints, bones, or deep subcutaneous tissues. More than half of soft tissue sarcomas develop in the arms or legs. About one in five (20%) are found in the abdominal cavity and present with symptoms similar to other abdominal-based health problems. The rest begin in the head and neck area (about 10%), and in and on the chest or abdomen (about 10%).1
There also are a vast number of non-malignant soft tissue neoplasms and tumors such as lipomas. Also typically included are cystic lesions of the deep tissues. The differentiating feature of soft tissue tumors (sarcomas) is that they arise from these connective tissues and do not arise from organs such as kidneys lungs, intestines, breasts, or thyroid glands.
Additional information on soft tissue sarcomas can be found in Weiss and Goldblum’s Enzinger and Weiss’s Soft Tissue Tumors, 5th ed.2
There are multiple soft tissue sarcomas with varying degrees of aggressive behavior, but virtually all have the capacity to metastasize and cause death. Treatment for high-grade soft tissue sarcomas is typically resection (removal) and radiation. Chemotherapy is playing an ever-increasing role, especially in high-grade (fast-growing) and metastatic cases.
The most common types of soft tissue sarcomas are described below.1 Cancer cells are often referred to as differentiated versus undifferentiated. Differentiation describes how much or how little tumor tissue looks like the normal tissue it came from. Well-differentiated cancer cells look more like normal cells and tend to grow and spread more slowly than poorly differentiated or undifferentiated cancer cells. Differentiation is used in tumor grading systems, which are different for each type of cancer.2
Malignant Fibrous Histiocytomas (MFH)/Pleomorphic Sarcomas (PS) Not Otherwise Specified (NOS)
The most commonly encountered soft tissue sarcoma is malignant fibrous histiocytoma, a tumor of the fibrous tissue most often occurring in the arms or legs. The least differentiated of the sarcomas, in many cases it represents a poorly defined, high-grade soft tissue sarcoma that cannot be further defined pathologically (histologically). A recent trend is to classify these poorly differentiated sarcomas as pleomorphic sarcomas or spindle cell sarcomas not otherwise specified, (NOS) rather than the previous designation as malignant fibrous histiocytoma. Poorly differentiated sarcomas typically affect older individuals. Analysis of annual rates of MFH and PS reflect this evolving diagnostic trend.
Liposarcomas
The next most commonly encountered and reported soft tissue sarcoma is liposarcoma, which is a malignant tumor of the fatty (adipose) tissues. This sarcoma also is more common in older persons. There are several subtypes ranging from the low-grade lipoma-like liposarcoma that rarely metastasizes to high-grade pleomorphic liposarcomas and round cell liposarcomas, which have a prognosis similar to malignant fibrous histiocytoma. Liposarcomas can develop anywhere in the body, but they most often develop in the thigh, around the knee, and inside the back of the abdomen. Seen in a wide range of patient ages, liposarcomas occur most frequently in adults between 50 years and 65 years old. Some liposarcomas grow very slowly, whereas others can grow quickly.
Synovial Sarcomas
The third most commonly encountered soft tissue sarcoma is synovial sarcoma, which is more likely to affect younger adults than previously mentioned sarcomas. The most common location is the thigh. Despite the name synovial sarcoma, most do not occur in joints or in the synovium of joints. It tends to occur mostly in young adults, but can also occur in children and in older people. Many of these cases respond very favorably to chemotherapy with significant shrinkage of the tumor, although resection (surgical removal) and radiation remain the cornerstones of current therapy. The prognosis is similar to malignant fibrous histiocytoma and the other high-grade soft tissue sarcomas mentioned above.
Tumors of Muscle Tissue
Leiomyosarcomas
Smooth muscle cells are found in internal organs such as stomach, intestines, blood vessels, or uterus. This muscle tissue gives these organs the ability to contract involuntarily. Leiomyosarcomas are malignant tumors of involuntary muscle tissue. They can occur almost anywhere in the body, but most often are found in the uterus. A second common site is the retroperitoneum (back of the abdomen) and in the internal organs and blood vessels where leiomyomas also arise. Less often, they develop in the deep soft tissues of the legs or arms. They tend to occur in adults, particularly the elderly. Since they often arise from arteries, resection of these tumors frequently requires an immediate vascular reconstruction.
Rhabdomyosarcomas
Skeletal muscles are the voluntary muscles that control and allow movement of arms and legs and other body parts. Rhabdomyosarcomas are malignant tumors of skeletal muscle. These tumors commonly grow in the arms or legs, but they can also begin in the head and neck area and in reproductive and urinary organs, such as the vagina or bladder. Rhabdomyosarcomas are primarily tumors of children. Clinically and behaviorally, they are in a class by themselves. They are treated with aggressive chemotherapy, as well as surgery and/or radiation in many cases. The aggressive treatments often cause permanent life-altering disability, even in survivors. For more information, see the American Cancer Society document "Rhabdomyosarcoma. [33]”
Malignant Peripheral Nerve Sheath Tumors
Malignant schwannomas, neurofibrosarcomas, or neurogenic sarcomas are malignant tumors of the cells that surround a nerve. The currently favored name for these sarcomas is malignant peripheral nerve sheath tumor.
Tumors of Blood Vessels and Lymph Vessels
Angiosarcomas
Malignant tumors can develop either from blood vessels (hemangiosarcomas) or from lymph vessels (lymphangiosarcomas). These tumors often develop in a part of the body that has been exposed to radiation. Angiosarcomas are sometimes seen in the breast after radiation therapy for breast cancer or in the arm on the same side as a breast that has been irradiated or removed by mastectomy. They are difficult to cure as they spread through the bloodstream to other parts of the body and often spread extensively through the local tissues.
Hemangiopericytoma
These are tumors of perivascular tissue (tissue around blood vessels). They most often develop in the legs, pelvis, and retroperitoneum (the back of the abdominal cavity) and are most common in adults. These can be either benign or malignant. They do not often spread to distant sites, but tend to recur where they started, even after surgery, unless widely excised. Following recent research and further histologic, genetic, and clinical evaluations, these have recently been reclassified as one end of the spectrum of malignant solitary fibrous tumors, or possibly identical to malignant solitary fibrous tumors.1
Hemangioendothelioma
This is a less aggressive blood vessel tumor than Hemangiosarcoma, but still considered a low-grade cancer. It usually invades nearby tissues, and sometimes can metastasize to distant parts of the body. It may develop in soft tissues or in internal organs, such as the liver or lungs.
Kaposi Sarcoma
These cancers are composed of cells similar to those lining blood or lymph vessels. In the past, Kaposi’s sarcoma was an uncommon cancer mostly seen in older people with no apparent immune system problems. It is now most common in people with human immunodeficiency virus (HIV) infection and the acquired immunodeficiency syndrome (AIDS), but can also develop in organ transplant patients who are taking medication to suppress their immune system. It is probably related to infection with a virus called human herpesvirus-8 (HHV-8).
Tumors of Fibrous Tissue
Fibrous tissue forms tendons and ligaments and covers bones, muscles and joint capsules, as well as other organs in the body.
Malignant fibrous histiocytoma (MFH)
MFH is found most often in the arms or legs. Less often, it can develop inside the back of the abdomen. This sarcoma is most common in older adults. Although it mostly tends to grow locally, it can spread to distant sites. It is the most commonly diagnosed soft tissue sarcoma, although now these are more often classified as pleomorphic sarcoma, not otherwise specified (NOS), as discussed above.
Fibrosarcoma
Fibrosarcomas are cancers of fibrous tissue. They have a characteristic herringbone cloth pattern when viewed under the microscope. Fibrosarcomas most commonly affect the legs, arms, or trunk. They are most common between the ages of 20 years and 60 years, but can occur at any age, even in infancy.
Dermatofibrosarcoma protuberans (DFSP)
These tumors are slow-growing cancers of the fibrous tissue beneath the skin, usually noted in the trunk or limbs. They invade nearby tissues but rarely metastasize. They primarily affect young adults. Due to their slow, insidious growth; their uncommon occurrence; and their innocuous appearance, diagnosis is often delayed. The local recurrence rate is higher than many sarcomas, and has been reported to be as high as 50% in some studies. While death due to disease is uncommon (<5%), the local recurrences can cause significant local morbidity.
Fibromatosis/Desmoid tumors
Fibromatosis is one of the names given to neoplastic tumors with features in between fibrosarcomas and benign tumors, such as fibromas and superficial fibrous diseases like Dupytren's disease. They tend to grow slowly, but often steadily. These tumors are often referred to as desmoid tumors. Although they do not metastasize, they do form in response to genetic alterations identical to many cancers and can cause great disability and even death. These tumors can invade nearby tissues, causing great havoc and occasionally even death. Some doctors may consider these to be a type of low-grade fibrosarcomas; most, however, regard these as benign but locally aggressive. Certain hormones, particularly estrogen, may increase the growth of some desmoid tumors. Antiestrogen drugs are sometimes useful in treating desmoids that cannot be completely removed by surgery. Radiation therapy plays a role in treatment, especially in unresectable or recurrent cases. There are ongoing chemotherapeutic trials in place with newer agents that interrupt the various biological processes in the growth of these tumors; these hold great promise for future patients. Additional research into the biology and treatment of these and virtually all tumors is clearly indicated.
Tumors of Uncertain Tissue Type
Through microscopic examination and other laboratory tests, doctors can usually find similarities between most sarcomas and certain types of normal soft tissues, thus, allowing them to be classified based on this histologic appearance. However, some sarcomas have not been linked to a specific type of normal soft tissue due to their unique appearance that does not closely resemble any single tissue type.
Malignant mesenchymoma
These very uncommon sarcomas contain areas showing features of at least two types of sarcoma, including fibrosarcomatous tissue per the original description. Since all connective tissue derive from undifferentiated mesenchymal tissues in an embryologic sense, it has been termed Mesenchymoma. The term has fallen out of favor and it is now thought that many cases may be better classified as one of the subtypes of sarcomas based on the tissue type contained within the tumor.3
Alveolar soft-part sarcoma
This rare cancer primarily affects young adults. The legs are the most common location of these tumors. This is one of the most vascular (blood vessels) sarcomas because it induces an extensive network of vessels to grow in and around the tumor. Because of their very slow growth rate, a delay in diagnosis can occur. Unfortunately, it ultimately has a high mortality rate and can lead to death years after diagnosis. The rate of progression can be quite slow; late metastases are common.
Epithelioid sarcoma
This sarcoma often develops in tissues under the skin of the hands, forearms, feet, or lower legs. Adolescents and young adults are often affected. These are often misdiagnosed as infections and chronic infectious ulcers because of their innocuous appearance and uncommon occurrence. This sarcoma has a much higher propensity for lymph node metastasis than most sarcomas, which usually preferentially metastasize to the lung.
Clear cell sarcoma
This rare cancer often develops in tissues of the arms or legs. It recently has been determined to be a variant of malignant melanoma, a type of cancer that develops from pigment-producing skin cells. How cancers with these features develop in parts of the body other than the skin is not known. As a melanoma, it behaves differently than sarcomas. It has a propensity to spread through the lymphatic system. Local recurrence is common; therefore wide resections are required for complete local eradication.
Other Types of Sarcoma
There are other types of soft tissue sarcomas, but they are less commonly encountered and not included in this discussion.
A recently published study, based on the National Cancer Database NCDB of the American College of Surgeons Commission on Cancers, reports the 13-year experience (1998–2010) with 34 of the most commonly encountered soft tissue sarcomas. This report provides a good overview of the US experience with these, including survival curves, the 2- and 5-year survivorship rate, and various demographic data. A current NCDB analysis of soft tissue sarcomas, including demographic data and survivorships are shown in Table 9A.9.1 to Table 9A.9.3. (Reference Table 8A.9.1 PDF [34] CSV [35], Table 8A.9.2 PDF [36] CSV [37], and Table 8A.9.3 PDF [38] CSV [39])
Soft tissue sarcomas account for less than 1% of all cancer cases diagnosed each year, and for a similar proportion of cancer deaths in a given year. Over the past decade, the overall incidence of soft tissue sarcomas showed a 31% increase in new cases diagnosed annually in the NCDB data, a slightly higher rate of increase than found for all the top 73 cancer sites reported. (Reference Table 8A.3.1 PDF [3] CSV [4] and Table 8A.5.2 PDF [9] CSV [10])
In terms of case numbers, the musculoskeletal health burden in the United States from soft tissue sarcomas is three to four times greater than that of bone and joint sarcomas. For the period from 2006 to 2010, the annual average number of soft tissue neoplasms, including the heart, approximated 14,000 cases/year in the SEER database, a number similar to those for Hodgkin lymphoma.1 Estimated new cases for 2014 by the American Cancer Society are 12,000.2 Soft tissue sarcomas come in a wide variety of forms that affect different age groups, but the most frequently encountered soft tissue sarcomas affect older adults. (Reference Table 8A.3.1 PDF [3] CSV [4])
As previously noted, the National Cancer Data Base (NCDB), a joint program of the Commission on Cancer and the American College of Surgeons, maintains the most thorough database on patients diagnosed with soft tissue sarcomas. Although the NCDB was not created to serve as an incidence-based registry, it currently gathers data on approximately 71% of the cancers treated in the United States. It should be noted this percentage varies from year to year based on the participation and reporting by hospitals to this voluntary database.
Over the 18-year period, 1985 to 2003, 86,355 soft tissue sarcomas of the extremities, shoulders ,and pelvic girdles and trunk were reported. This number excludes approximately 32,250 soft tissue sarcomas of the head and neck, thoracic, and abdominal areas; these patients are generally cared for by non-musculoskeletal specialists. Using a 20-year average and assuming 70% of the annual US cases are included in NCDB, more than 5,700 new cases of soft tissue sarcoma would have occurred annually. This compares to the estimated 12,020 cases predicted for 2014 by the American Cancer Society.2
A 2014 report by Corey, Swett, and Ward examined the adult cases reported to the NCDB of soft tissue sarcomas over a 13-year interval (1998–2010). In 2010, 5,070 soft tissue sarcomas were reported to the NCDB. While the numbers of soft tissue sarcomas reported to the NCDB increased by 19% over this 13-year period, the number of bone sarcomas reported to the NCDB increased by only 10.7% during this same time period.3
While soft tissue sarcomas can be found among all ages, the incidence increases after the age of 55 years. Once a person reaches age 85 years or older, the incidence of diagnosis drops sharply. Males are diagnosed with soft tissue sarcomas at a slightly higher age than females. Blacks are diagnosed an average of 10 years earlier than those who are White. (Reference Table 8A.3.1 PDF [3] CSV [4], Table 8A.3.2 PDF [17] CSV [18], and Table 8A.2.1 PDF [15] CSV [16])
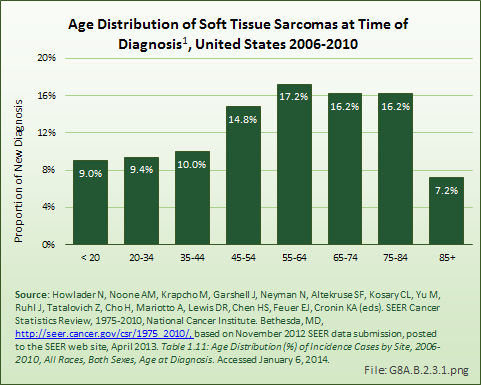
The age distribution at time of death for persons diagnosed with soft tissue sarcomas reflects a relative survival rate that favors younger persons. (Reference Table 8A.3.4 PDF [43] CSV [44])
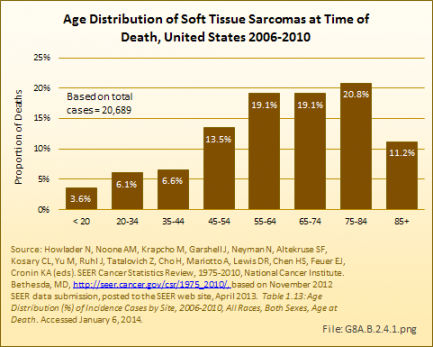
The 5-year survival rate for soft tissue sarcomas is reported at 66% by both the SEER database and the National Cancer Institute (NCI). This is a rate similar to that for bone and joint, uterine/ovarian, and non-Hodgkin lymphoma cancers. Average length of survival after diagnosis is 7 years, similar to that of breast, urinary, and nervous system cancers. White women have a slightly higher 5-year survival rate than do men, and live an average of 1 year longer after diagnosis. However, the reverse is true for Black women, who die an average of 2 years sooner than Black men diagnosed with soft tissue sarcoma. (Reference Table 8A.4.1 PDF [23] CSV [24], Table 8A.4.2 PDF [25] CSV [26], and Table 8A.4.3 PDF [21] CSV [22])

For high-grade soft tissue sarcomas, the most important prognostic factor is the stage at which the tumor is identified. Staging criteria for soft tissue sarcomas are primarily determined by whether the tumor has metastasized or spread elsewhere in the body. Size is highly correlated with risk of metastasis and survival. In general, the prognosis for a soft tissue sarcoma is poorer if the sarcoma is large. As a general rule, high-grade soft tissue sarcomas over 10 cm in diameter have an approximate 50% mortality rate and those over 15 cm in diameter have an approximate 75% mortality rate.
The NCI statistics staging classification of sarcomas is Stage 1, confined to the primary site (localized: 54% of sarcomas are diagnosed at this stage); Stage 2, spread to regional lymph nodes or directly beyond the primary site (regional: 22%); or Stage 3, metastasized (distant: 15%). For the remaining cases, the staging information was unknown. The corresponding 5-year relative survival rates reported are 84% for localized sarcomas, 62% for regional stage sarcomas, 16% for sarcomas with distant spread, and 54% for unstaged sarcomas. The 10-year relative survival rate is only slightly worse for these stages, meaning that most people who survive 5 years are cured.1
Using the staging criteria of soft tissue sarcomas of the American Joint Committee on Cancer (AJCC) produces similar results for sarcomas found in the limbs (arms or legs): 90% 5-year survival rate for Stage 1 sarcomas; 81% for Stage 2; and 56% for Stage 3. Sarcomas identified as Stage 4 have a very low 5-year survival rate. Sarcomas located in other than a limb also have lower survival rates.1
Sarcomas are often staged by orthopedic oncologists with a staging system established by Dr. William Enneking, and adopted and modified by surgical societies primarily consisting of orthopedic oncologists. That may have accounted for the lack of AJCC staging data in many cases of bone and soft tissue sarcomas reported to the NCDB. Nearly 40% of cases for 2000–2011 reported in the NCDB data have an unknown stage. This is a much higher proportion than found among other common cancer types, making it difficult to compare the severity of soft tissue sarcomas to other cancers. However, none of the cases was identified as Stage 1, with the majority at Stage 2 through Stage 4. (Reference Table 8A.5.1 PDF [45] CSV [46])
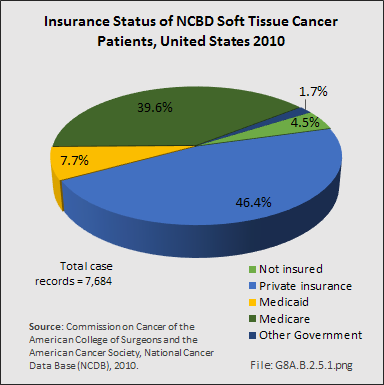
From 1998–2010, information on insurance coverage was available for roughly 96% of patients treated with soft tissue sarcomas. The largest insurance payer was managed care (33%), followed by Medicare with supplement (25%). Private insurance accounted for 14%, while Medicare (11%) accounted for a larger percentile than Medicaid (5%). Detailed NCDB insurance data for 7,684 of 7,878 cases of soft tissue sarcoma reported from the year 2010 showed private insurance paying just over 46%, while Medicare/Medicaid paid a slightly larger share of 47%.1
The total economic costs of malignant soft tissue sarcoma are unknown. Surgery is often the first line of treatment for soft tissue sarcoma. Multiple therapies may be needed later in the course of the patient’s disease, especially in the more advanced cases. In the later stages of the disease in those not cured with surgery alone, significant costs will accumulate as the patients develop pulmonary disease and ultimately die. Hormone therapy, immunotherapy, and bone marrow transplant/endocrine treatments are undertaken in a small number of cases that fail standard treatments. Overall, costs will vary with treatments utilized, number and intensity of treatments, and can easily top $100,000 for a single patient that receives surgery, chemotherapy, and radiation therapy.
Throughout the years 2005–2008, one study reported that the average professional charge for a primary excision was $9,700 and $12, 900 for re-excision. Although every 1-cm increase in size of the tumor results in an increase of $148 for a primary excision, size was not an independent factor affecting re-excision rates. The grade of the tumor was positively associated with professional charge, such that higher-grade tumors resulted in higher charges compared to lower-grade tumors. Analysis including professional technical and indirect charges revealed that, on average, patients undergoing definitive primary excision at their cancer treatment center were charged $40,230. This was compared to $44,770 for to patients receiving definitive re-excision of unsuccessful or incomplete previous resections at the same cancer treatment center. This higher cost did not include the charges and costs generated by their previous unsuccessful or incomplete previous attempt at resection.2
This analysis confirms that proper work-up, evaluation, and treatment are key to maintain costs, as well as, hopefully, improving the outcome for these patients. This cost analysis did not include the costs associated with chemotherapy or radiation therapy, or the costs of diagnostic and follow-up laboratory and radiographic studies, nor the actual costs of care.
The majority of sarcomas develop in people with no known risk factors: There is currently no known way to prevent these cases at this time. Whereas future developments in genomic research may allow genetic testing to identify persons with increased risk to develop soft tissue sarcomas, few such predictors are available at present. Reporting suspicious lumps and growths or unusual symptoms to a doctor, and appropriate evaluation of such abnormalities can help diagnose soft tissue cancer at an earlier stage. Treatment is thought to be more effective when detected early, as smaller-diameter sarcomas have been shown to have improved outcome compared to large sarcomas.
Cancers occasionally spread or metastasize to the soft tissues, such as the muscles and deep tissues of the body, including the thigh and leg. The most likely cancers to do so are cancers of the lung and kidney. As such, this fact must always be borne in mind whenever physicians examine a patient presenting with a new mass in the leg, thigh, or other soft tissues, especially if they have a history of a prior lung or kidney cancer.
Links:
[1] https://www.boneandjointburden.org/docs/T8A.1.1.pdf
[2] https://www.boneandjointburden.org/docs/T8A.1.1.csv
[3] https://www.boneandjointburden.org/docs/T8A.3.1.pdf
[4] https://www.boneandjointburden.org/docs/T8A.3.1.csv
[5] https://www.boneandjointburden.org/docs/T8A.3.3.pdf
[6] https://www.boneandjointburden.org/docs/T8A.3.3.csv
[7] http://seer.cancer.gov/seerstat/
[8] https://www.facs.org/quality%20programs/cancer/ncdb
[9] https://www.boneandjointburden.org/docs/T8A.5.2.pdf
[10] https://www.boneandjointburden.org/docs/T8A.5.2.csv
[11] http://seer.cancer.gov/statfacts/html/bones.html
[12] http://seer.cancer.gov/statfacts/html/mulmy.html
[13] https://www.boneandjointburden.org/docs/T8A.1.2.pdf
[14] https://www.boneandjointburden.org/docs/T8A.1.2.csv
[15] https://www.boneandjointburden.org/docs/T8A.2.1.pdf
[16] https://www.boneandjointburden.org/docs/T8A.2.1.csv
[17] https://www.boneandjointburden.org/docs/T8A.3.2.pdf
[18] https://www.boneandjointburden.org/docs/T8A.3.2.csv
[19] https://www.boneandjointburden.org/docs/T8A.2.2.pdf
[20] https://www.boneandjointburden.org/docs/T8A.2.2.csv
[21] https://www.boneandjointburden.org/docs/T8A.4.3.pdf
[22] https://www.boneandjointburden.org/docs/T8A.4.3.csv
[23] https://www.boneandjointburden.org/docs/T8A.4.1.pdf
[24] https://www.boneandjointburden.org/docs/T8A.4.1.csv
[25] https://www.boneandjointburden.org/docs/T8A.4.2.pdf
[26] https://www.boneandjointburden.org/docs/T8A.4.2.csv
[27] https://www.boneandjointburden.org/docs/T8A.8.1.pdf
[28] https://www.boneandjointburden.org/docs/T8A.8.1.csv
[29] http://www.cancer.net/cancer-types/osteosarcoma-childhood/statistics
[30] http://www.cancer.net/cancer-types/ewing-sarcoma-childhood/statistics
[31] http://seer.cancer.gov/statfacts/more.html.
[32] http://www.cancer.org/cancer/sarcoma-adultsofttissuecancer/detailedguide/sarcoma-adult-soft-tissue-cancer-soft-tissue-sarcoma
[33] http://www.cancer.org/cancer/rhabdomyosarcoma/detailedguide/rhabdomyosarcoma-detailed-guide-toc
[34] https://www.boneandjointburden.org/docs/T8A.9.1.pdf
[35] https://www.boneandjointburden.org/docs/T8A.9.1.csv
[36] https://www.boneandjointburden.org/docs/T8A.9.2.pdf
[37] https://www.boneandjointburden.org/docs/T8A.9.2.csv
[38] https://www.boneandjointburden.org/docs/T8A.9.3.pdf
[39] https://www.boneandjointburden.org/docs/T8A.9.3.csv
[40] http://www.cancer.gov/dictionary?cdrid=46445
[41] http://www.facs.org/cancer/ncdb/publicaccess.html
[42] http://www.cancer.org/cancer/sarcoma-adultsofttissuecancer/detailedguide/sarcoma-adult-soft-tissue-cancer-key-statistics
[43] https://www.boneandjointburden.org/docs/T8A.3.4.pdf
[44] https://www.boneandjointburden.org/docs/T8A.3.4.csv
[45] https://www.boneandjointburden.org/docs/T8A.5.1.pdf
[46] https://www.boneandjointburden.org/docs/T8A.5.1.csv
[47] http://www.cancer.org/cancer/sarcoma-adultsofttissuecancer/detailedguide/sarcoma-adult-soft-tissue-cancer-staging